Weight Loss Surgery: Everything You Need to Know [2021]
Overweight is really a big problem that affects every aspect of your life negatively. Let it be a party with friends, hanging out with them, or any activity related to sports.
Being overweight will hinder these activities, thus creating barriers to happiness. If you are also suffering from this problem, it’s granted that you want to fight it in any way and want to overcome it. Which is of course a rational decision.
However, there are many ways to lose weight. Doing an exercise or following a healthy diet. In this article, we are going to discuss the Surgery method of weight loss.
If you are currently considering any form of weight loss surgery, it is likely that you have been thinking about your decision for some time.
Certainly, it is a decision that warrants much thoughtful consideration. Hopefully, this article will help you with various aspects of your decision-making process.
Also Read: Best WEIGHT LOSS HACKS for You!
Perhaps you began to think about weight loss surgery after a conversation with your primary care physician, who was concerned about specific obesity-related health problems, such as heart disease, hypertension, high cholesterol, diabetes, or sleep apnea.
Perhaps as weight-loss surgeries of various types got more media coverage, you learned more about one or more of the procedures and thought that some form of weight loss surgery might be right for you. Possibly, a friend or relative has already undergone weight loss surgery.
Or maybe you just began to research it on your own after years of struggling with more traditional methods of weight loss, typically involving dieting and exercise.
In any case, you’ve obviously begun to think seriously about having surgery to correct your weight problem once and for all, or you wouldn’t be reading this.
The decision to pursue weight loss surgery should not be taken lightly. There are many factors to consider.
A person who has made the decision for weight loss surgery must know a great deal of information as it’s not something that should be taken lightly.
This article contains all the need-to-know information about weight loss surgery and how to decide whether or not it is right for you.
It will help guide you through the decision-making process by providing information on the various types of bariatric surgery available, their respective risks and benefits, the professional consultations and evaluations you will need to undergo prior to surgery, and what to expect postoperatively.
The following issues should be taken into account as you consider whether or not weight loss surgery is right for you.
Also Check: Best Way to Lose up to 50 Pounds
Contents
Your Body Weight

First, do you qualify for the diagnosis of severe obesity? This is one of the first considerations when deciding if surgery is an appropriate weight-loss tool for you. Doctors use the body mass index (BMI) to categorize degrees of overweight in patients.
You can calculate your BMI as follows:
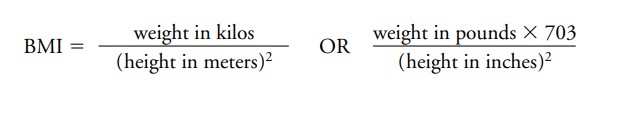
A BMI of 20–25 is considered normal, 25–30 overweight, and over 30 obese. However, surgery is not recommended as a weight management tool unless your BMI is over 40 or is over 35 and you have other significant health problems.
If your BMI is under 35, that is wonderful news! This means that you are at significantly less risk from being overweight and no longer need to consider surgery, as other weight loss methods may well succeed and will carry less risk.
Over 40 BMI
If your BMI is over 40, you are severely, or morbidly, obese, and surgery may be an option worth considering.
In the few studies that have examined weight loss surgery and compared it to traditional weight loss methods, bariatric surgery seems to result in greater weight loss over time in patients who are significantly overweight.
A description of the different types of surgeries and more detail on the research is given in the following sections.
BMI 35-40
If your BMI is between 35 and 40, or if you haven’t had a good health screening in a while, the next step is to assess your overall health, paying particular attention to conditions that result primarily from or are greatly exacerbated by being overweight. It is important to ask your doctor for a comprehensive history and exam.
Some overweight patients hate to go to the doctor because they feel self-conscious and sometimes even feel that the doctor’s office is not a friendly place.
If this is the case, be sure to ask friends to recommend a doctor you feel comfortable with and trust. You deserve to have a provider you enjoy seeing.
Considering bariatric surgery is a big step and it will help if you can discuss it openly with your physician.
Medical Concerns

Cardiac Risk
Hyperlipidemia is a common complication of obesity. Studies have shown coronary artery disease, evidenced by plaques in the blood vessels extending from the heart, occurring as early as late adolescence.
They have also shown that high LDL (“bad”) cholesterol, low HDL (“good”) cholesterol, and high triglycerides are common factors accompanying the development of coronary artery disease.
As a result, all obese adults should be screened for lipid or cholesterol abnormalities. Lifestyle changes are often the first line of therapy against abnormal lipids in the blood.
Hypertension is also increasingly recognized as a common side effect of obesity. Weight loss can produce dramatic improvements in blood pressure.
If you have been diagnosed with obesity, hypertension, and hyperlipidemia, you may also have “metabolic syndrome.” This is a newly described clustering of metabolic risk factors, known to have a significant negative effect on heart health.
The factors include abdominal obesity, low HDL, high triglycerides, insulin resistance or diabetes, and high blood pressure.
All these factors are thought to be caused by insulin resistance, a condition in which the body becomes increasingly resistant to the actions of insulin, a hormone secreted by the pancreas.
If you have had chest pain or shortness of breath your doctor may have tested you for the possible presence of arteriosclerosis, or coronary artery disease.
If you have noticed any of these symptoms and have not told your doctor, you should call him or her immediately, as they can be signs of serious illness.
If you have had a heart attack, stroke, or congestive heart failure, you have certainly been told that your weight may be contributing to your poor heart health.
Type 2 Diabetes/Glucose Intolerance
The incidence of type 2 diabetes in the United States is rising dramatically, paralleling the rise in obesity. Obesity is a known contributor to the development of type 2 diabetes.
Other risk factors include a positive family history of NIDDM (noninsulin-dependent diabetes), increased body fat and abdominal fat, insulin resistance, and ethnicity (with greater risk in African American, Hispanic, and Native American adults).
Heart disease, vision problems, kidney failure, high blood pressure, and stroke can complicate NIDDM. Because NIDDM can lead to premature death and disability, addressing excess weight in people with type 2 diabetes is critical.
Polycystic Ovary Syndrome and Menstrual Irregularities
First of all, ovarian cysts are normal variants for many women. Having cysts on your ovaries does not mean you have polycystic ovary syndrome (PCOS).
Many women suffer from PCOS, which is characterized by menstrual changes, acne, or excessive hair growth (on the face, abdomen, chest, and back)—signs of hyperandrogenism, or excessive male hormones.
About 50–75% of women with PCOS are obese, and obesity may be a factor in the development of PCOS in some susceptible women.
If you have been diagnosed with PCOS and are obese, you have an elevated risk of developing hyperlipidemia, hypertension, diabetes, and metabolic syndrome.
It may also be especially hard for you to lose weight because many women with this syndrome have abnormalities in insulin metabolism.
To complete this negative health cycle, obesity seems to contribute to the insulin resistance and risk for diabetes that many women with PCOS experience.
Pulmonary Risk and Obstructive Sleep Apnea
Obstructive sleep apnea (OSA) is common among the extremely obese. This condition has a known link to future cardiovascular disease and can be fatal.
Current recommendations state that all overweight adults should be screened for snoring, and those who snore should have a sleep study including a polysomnogram to determine if they have OSA.
Many overweight individuals are diagnosed with asthma. Obesity is certainly one of many factors that can worsen symptoms of asthma.
However, sometimes shortness of breath indicates that there is either undiagnosed heart disease or that extra weight is making it harder for the lungs to do their job every day.
This is not asthma but restrictive lung disease. It is helped not by inhalers but by weight loss. So if you have shortness of breath and you haven’t talked to your doctor, make sure to do so to clarify the specific cause is, whether or not you already know you have asthma.
Gastrointestinal Problems
Many kinds of gastrointestinal problems can occur in significantly overweight people. Nonalcoholic fatty liver disease (NAFLD) is currently the most common cause of abnormal liver tests in the United States. It is commonly seen in association with obesity, diabetes, hypertension, and hypertriglyceridemia.
Most patients have no symptoms and present only with mildly abnormal laboratory results. It is not clear how NAFLD develops, but it can progress to hepatitis, cirrhosis, and end-stage liver disease.
In one study examining the liver biopsies of morbidly obese adults preparing to undergo gastric bypass surgery, 65% of the patients had moderate to severe liver changes, 12% had advanced fibrosis or scarring of the liver, and 33% had nonalcoholic hepatitis.
The presence of type 2 diabetes was strongly correlated with advanced liver disease, more so than was BMI.
Gastrointestinal reflux, or heartburn, is a common but bothersome condition that is often exacerbated by weight.
Reflux can cause chest pain, an acid taste in the mouth, and a cough, among other symptoms. Fatty foods, cigarettes, alcohol, caffeine, and certain medications can worsen it.
While reflux can often be managed medically, it can sometimes lead to changes in the esophagus that can predispose one to cancer.
Finally, nearly 50% of cases of gallstones, small stones that can obstruct the normal flow of bile from and within the gall bladder, are associated with obesity.
Gallstones can impede efforts at weight loss. Also, gallstones can sometimes be a complication of weight loss surgery as well.
Be on the lookout for this condition, which often causes periodic abdominal pain, particularly if you have a family history of gall bladder disease, in order to get diagnosed and treated early.
Orthopedic Complications
Overweight adults are at increased risk for a number of weight-related orthopedic complications.
Chronic excess weight can lead to a bowing of the lower legs called Blount’s disease. Significant hip, knee, and back pain, and even osteoarthritis can result from the excess pressure on joints that increased body mass imposes.
Many overweight patients require hip and knee replacements that, while effective, are costly and time-consuming interventions to manage pain and improve range of motion. Significant weight loss is known to help with such orthopedic diseases.
Idiopathic Intracranial Hypertension (Pseudotumor Cerebri)
Idiopathic intracranial hypertension (IIH), also known as pseudotumor cerebri, is a condition seen much more commonly in obese individuals.
As its name implies, IIH is associated with increased intracranial pressure in the absence of tumors or other brain diseases.
It often causes severe headaches and can sometimes lead to blindness. To diagnose IIH, your doctor will need to do a careful eye exam and perhaps even use magnetic resonance imaging (MRI) and a spinal tap, or lumbar puncture, to check the pressure of your spinal fluid. Once diagnosed, IIH requires that you promptly lose weight.
Genitourinary Conditions
Many overweight women experience stress incontinence, a condition that can cause mild to severe leakage of urine from the bladder when they sneeze, laugh, cough, or even go for a walk.
The condition develops when the abdomen increasingly exerts pressure on the bladder. Although surgery and medications can help control the problem, they often fail to. Weight loss can often significantly relieve symptoms.
Gout is caused by a buildup of uric acid that exceeds what the kidneys can filter. The acid builds up in the joints and can cause swelling, inflammation, and pain, most commonly in the big toe or ankle joints.
Obesity increases the risk of developing gout, as does alcohol consumption, a diet high in uric acid (red meat, red wine, cream sauces), and kidney failure. Recent studies describe links between gout and high blood pressure as well.
While gout is best managed with dietary changes and medication, weight loss will help prevent its recurrence.
Skin and Blood Vessels
Often, overweight patients notice that areas of hanging skin folds, particularly around the breasts, abdomen, and inner thighs, can become chafed, irritated, and difficult to clean.
Superficial fungal or bacterial infections of the skin can result and can lead to deep tissue infections, although this is rare.
Patients who are extremely obese, especially those with diabetes, tend to have decreased circulation to their hands and feet, delaying the healing of such infections.
Obese individuals often develop venous stasis, wherein slowed blood flow to the legs’ veins leads to damage to the valves in the leg veins.
Obesity can worsen this condition by making it hard to maintain regular mobility: a sedentary lifestyle further inhibits blood flow.
Especially in those with a family history of venous stasis, this can lead to superficial varicose veins, a benign but unattractive condition.
A separate, more serious complication of venous stasis is deep venous thrombosis (DVT), a blood clot in a deep leg vein.
These clots need to be promptly managed, as they can lead to life-threatening complications such as pulmonary embolism. Leg swelling and pain can indicate DVT.
Cancer
Cancer risk increases with obesity. It is unclear whether weight loss can decrease the risk. Cancers associated with weight gain are those of the prostate, colon, breast, uterus, and gall bladder.
Also Check: Gucci Mane Weight Loss
Other Issues to Consider Before Surgery
Once medical illnesses and risks have been examined thoroughly, it is important to examine your history of dieting attempts, unhealthy eating patterns and substance abuse habits, and emotional issues before proceeding with surgery.
Dieting History
Discuss with your therapist your dieting experiences and how these experiences have affected your decision to undergo weight loss surgery.
Have you made concerted efforts over a period of several months to a year or more to try to follow one or more traditional, medically supervised weight control programs such as a modified fast (Opt fast, Medifast), Weight Watcher’s, a dietician-prescribed low-calorie diet, diet medications (Phen-fen, Meridia, Xenical, Redux), Jenny Craig, or Nutrisystem,
Or other weight loss programs such as Atkins, Slim-Fast, calorie counting plus exercise, and the like? If so, how many times have you tried to diet, and for how long each time? How many pounds have you been able to lose each time, and how long were you able to keep the weight off?
If you are a teenager, your parents can offer doctors much important information about your weight and eating history.
Often, weight gain starts quite young, and early eating and feeding patterns can be important in understanding how your body uses and stores energy.
You should therefore expect that your parents will be asked to meet with your doctors, and you should be appreciative of their involvement in the process, even though it may, at times, seem to be the opposite of what you want.
Emotional Issues
It is important to examine your emotional life, both current and past, and of course to discuss any emotional issues with your therapist as you prepare yourself to make a decision about surgery.
For obvious reasons, it is important that you are in a positive frame of mind when you undergo surgery.
This means that you must not be suffering from serious depression, particularly depression that prevents you from being up, active, and optimistic about your life situation.
If you are experiencing sadness or a low mood and have difficulty enjoying pleasant events and activities, or if you have had trouble getting up in the morning, are easily distracted, have poor concentration, are fearful, or have thought or planned to harm yourself or end your life, you are too depressed to proceed with surgery at this time.
Similarly, anyone with significant anxiety (e.g., worries that prevent you from leaving the house, interacting comfortably with other people, or tolerating various types of fairly common daily experiences) will probably be ruled out for surgery until the anxiety can be better controlled.
Trauma
Many people who become obese have histories of traumatic experiences of one type or another, and these issues should be addressed in some form of therapy or counseling before weight loss surgery is seriously considered or the preparation process has begun.
Other Problematic Eating Behaviors

While some obese individuals report problematic eating behaviors such as out-of-control binge eating, eating a lot very late at night, grazing throughout the day, or taking in excessive amounts of regular soda, many reports simply eating too much at regular meals and snacks and exercising too little.
If you have a problem with binge eating, it definitely needs to be addressed before surgery for a number of reasons.
Binge eating is defined as eating a large amount of food (e.g., more than others would consume in a similar circumstance) in a small amount of time in a manner that feels “out of control” or irresistible and impossible to interrupt.
Some people who binge report a sense of “spacing out” or dissociating while they are eating.
For example, while eating, they might be able to block out their thoughts and feelings in full or to some degree, making overeating a seemingly “great escape” from all types of distress.
About half of those who are obese have problems with binge eating. If you frequently binge (perhaps in addition to other forms of overeating), it is best that you try to resolve that problem before undergoing surgery.
Procedure: What you Need to Know
Currently, there are a few popular procedures. Some are only restrictive in nature, meaning that a new, smaller stomach “pouch” is created and the exit of food from the stomach is limited (slowed gastric emptying), and some are also malabsorptive, meaning that the surgery changes how food is absorbed as it leaves the stomach and enters the small intestine, usually because part of the small intestine is rerouted or removed.
Some surgeries lead to more rapid weight loss and more complications. Some procedures are “open,” meaning that they require a larger abdominal incision; some can be laparoscopically performed, with the surgeon—at some centers assisted by a robot—operating via a camera that goes through a small incision; and some surgeries can be performed either way.
The surgeries that are the best-studied, most accepted, and most commonly performed are the laparoscopic adjustable-silicone gastric banding (lap-band) and the roux-en-Y gastric bypass (RYGB). Some surgeons still perform a biliopancreatic diversion, although many consider this surgery to be on the decline because of the higher rates of complications and technical difficulties.
Risks and Benefits
Each surgery has its own risks and benefits. I will describe common complications and nutritional deficiencies reported with each surgery.
Unfortunately, the quality of the research done on weight loss surgery has been suboptimal, although it has improved in recent years.
In 2005 the Cochrane group published an updated review and analysis of all the literature to date on weight loss surgery, attempting to identify the effects of surgery for morbid obesity on medical illness, weight, and quality of life.
This analysis identified only 26 studies out of 3,223 published references as being of high enough quality to use in their report, and most of these 26 studies still contained much bias, according to the reviewers.
This does not mean that the publications were invalid but simply that they are preliminary and often do not compare different surgical approaches to each other or to other weight loss methods, did not use appropriate research procedures to “randomize” patients (necessary for comparing different approaches), and/or did not follow patients for a long enough period of time (at least 12 months) to be able to detect long-term effects.
What it does mean is that despite a lot of research on obesity surgery, there are many things that doctors still do not know and need to learn, and you should consider this fact.
Like any other significant medical procedure, there are known risks, and in this field, there may be additional risks that are not yet understood by the medical community.
Make sure to thoroughly consider this when making your decision, and to discuss it with your physicians, as you are the only person who can assess how much risk you are comfortable with.
Surgical Procedures
Restrictive Procedures
Vertical Banded Gastroplasty (VBG)
In this procedure, the stomach is divided by a line of staples to produce a much smaller gastric pouch that holds only about an ounce.
The outlet of the new pouch is similarly small, about 10–12 mm in diameter. This outlet empties into a section of the stomach that then empties, as before, into the small intestine.
The surgeon usually reinforces the outlet with mesh or Gore-Tex. The VBG may be performed with an open incision or laparoscopically.
Siliastic-Ring Vertical Gastroplasty
A variant of the gastroplasty described above. Here, the stomach is again divided by a row of staples to produce a small gastric pouch.
In this procedure, the new, smaller outlet of the new gastric pouch is reinforced by a silicone band to produce a narrow exit into the stomach, as detailed above.
Laparoscopic Adjustable Silicone Gastric Banding (LASGB)
This surgery, known as the lap-band, was approved by the U.S. Food and Drug administration in 2001. It is performed only laparoscopically, as its name indicates.
Here, a new gastric pouch is formed with staples, as with the gastroplasty, but the band surrounding the outlet from the new pouch into the stomach is adjustable because the band is connected to a reservoir that is implanted under the skin.
The surgeon can inject saline into the reservoir, or remove it from the reservoir, in an outpatient setting to tighten or loosen the band, thereby adjusting the size of the gastric outlet.
Restrictive Malabsorptive
Roux-en-Y Gastric Bypass (RYGB)
The RYGB is the most commonly performed procedure. It involves creating a small (1/3-1 oz) gastric pouch by either separating or stapling the stomach.
This pouch drains via a narrow passageway to the middle part of the small intestine, the jejunum, bypassing the duodenum, through which food normally traverses before arriving at the jejunum.
The older portion of the stomach goes unused and maintains its normal connection to the duodenum and the first half of the jejunum.
This end of the jejunum is then attached to a “new” small intestine created by the procedure above. This forms the “Y” referred to in the name of the procedure.
This redirection of the small intestine is a malabsorptive feature complementing the restrictive feature that is the smaller gastric pouch. RYGB may be performed with an open incision or laparoscopically.
Biliopancreatic Diversion (BPD)
This surgery is considered more technically difficult and so is less commonly performed.
It involves a gastrectomy that is considered “subtotal,” meaning it leaves a much larger gastric pouch compared with the options described above.
The small intestine is divided at the level of the ileum (the third and final portion of the small intestine), then the ileum is connected directly to this midsize gastric pouch.
The remaining part of the small intestine is then also attached to the ileum. This procedure thereby bypasses part of the stomach and the entire duodenum and jejunum, leaving only a small section of the small intestine for absorption.
Biliopancreatic Diversion with Duodenal Switch (BPDDS)
This is a variation of BPD. It preserves the first portion of the duodenum, the first section of the small intestine.
Jejunoileal Bypass
This surgery bypasses large portions of the small intestine; it is no longer recommended in the United States and Europe because of the high rate of complications and mortality.
Think twice about trusting a physician who treats the idea of obesity surgery lightly, as if it is no big deal or your only option, as this is not a reasonable conclusion to draw from what we know.
Surgery might be an appropriate option for you, especially if you have endured years of poor health, poor quality of life, low self-esteem, and social stigmatization because of extreme obesity and have made multiple unsuccessful attempts to lose weight using other methods.
A good, experienced surgeon will be the first to admit that there are risks from the surgery and these should be considered along with the benefits when determining whether bariatric surgery is right for you.
First, it is important to remember that this is a surgical procedure, done under general anesthesia, and therefore certainly carries a risk of complications, including possible death.
The rate of each risk varies with the age, health, and weight of the patient and with the type of surgery.
Morbidly obese patients are considered “high-risk” patients for surgery because a higher dose of anesthesia is used, the surgery is more difficult to perform, and their overall health is often poor, increasing the likelihood of possible complications.
However, data from the International Bariatric Surgery Registry—a registry of more than 10,000 patients—reveals a 30-day mortality rate of 0.3%.
Other published studies have shown 30-day mortality rates of anywhere from 0.2% to 1.9%. One study of Medicare beneficiaries (who are thought to have potentially poorer overall health) showed a 30- day mortality of 2.0% and a one-year mortality rate of 4.6%.
Mortality rates are higher in older patients, especially those older than 65 at the time of surgery.
The experience of your surgeon has a major effect on both mortality rates and rates of re-hospitalization in the years following surgery.
Studies show a direct correlation between the surgeon’s caseload (how many bariatric surgeries he or she performs regularly, which usually also reflects his or her experience level), and lower mortality and re-hospitalization rates.
You should choose a doctor who is board-certified in surgery and who is a member of the American Society for Bariatric Surgery.
Choosing a Surgeon
After meeting with your PCP and getting the go-ahead from him or her, you will need to locate a surgeon with whom you want to work, who is available to work with you, and who may be covered by your health insurance.
Ask your PCP for referrals, speak to others in your area who have already undergone weight loss surgery or are considering it, look up resources on the Internet using such search terms as “weight loss surgery,” or request the names of qualified surgeons in your area from national associations, such as an association of weight loss surgeons or other obesity specialists.
Once you identify potential surgeons, research their credentials. For example, you will want to know the number of weight loss surgery procedures they have done, whether or not they are board-certified, whether or not they have ever been sued for negligence or malpractice, and how they have been evaluated by other patients in terms of surgical skill, bedside manner, and the like.
Once you select a surgeon and schedule a meeting with him or her, you should be prepared for any of the following.
The meeting with your surgeon might take place before or after you see the various other health professionals involved in the preoperative screening process, depending on the policies of the particular center you are working with.
Either way, it is likely you will feel some anxiety before meeting the surgeon—this is normal under the circumstances.
The following information can help you counter that anxiety and feel more comfortable and relaxed when you do meet your surgeon for the first time.
Question Your Surgeon May ask
Your appointment will probably take place in some kind of clinic or doctor’s office. Your surgeon will likely ask questions about your current physical and mental health and your health history, your successful and unsuccessful attempts at dieting, and your exercise habits.
He or she will try to get some sense of your rationale for considering surgery at this time and attempt to determine your current state of mind to ascertain whether or not you are psychologically ready to undergo the procedure.
In considering your state of mind, he or she may ask you specific questions about your mental health and drug and alcohol use and general questions about your lifestyle, including habits such as smoking and exercise.
The surgeon will also ask about your eating habits including any particular eating problems such as binge eating, eating late at night, drinking excessive amounts of soda or other fluids, and so on.
Much of this information will be supplemented with records that the surgeon has obtained from your PCP (such as a letter referring you to the weight loss surgery program, lab results, and/or your entire medical record) and the other health professionals that you may have consulted before meeting with your surgeon.
A Comprehensive Checklist

The following checklist can help you keep track of where you are in terms of these numerous preoperative requirements.
Your diary or journal will also prove useful to help you keep track of the process. Following the checklist are discussion questions and exercises to help you get in touch with several of the crucial issues related to your surgery.
Have you:
1. Found a program you like?
2. Identified a surgeon with whom you are comfortable, who has accepted you as a patient and offered the weight loss procedure that you want?
3. Been referred to this program and surgeon by your primary care physician (PCP)?
4. Determined if your insurance will cover the surgery, or found other financings?
5. Met with a program-endorsed:
- a. Dietician?
- b. Mental Health Professional?
- c. Internist?
- d. Gastroenterologist?
6. Followed through with the professionals’ recommendations:
- a. To keep records such as food and exercise logs?
- b. To start to lose weight and/or exercise, if this is required?
- c. To begin to recondition yourself in preparation for surgery (e.g., improve eating patterns, nutrition, activity level), if weight loss is not required?
- d. To start counseling, therapy, or medication treatment for a mood issue?
- e. To begin any other necessary medication or treatment (such Continuous Positive Airway Pressure [CPAP] for sleep apnea)?
- f. To make follow-up visits with the dietician, if this was recommended?
7. Begun to think at a deeper level about the experience of undergoing a radical surgery, to emotionally prepare for the surgery, and to discuss these issues with significant others or other members of your support network? This work should include:
- a. Getting in touch with your feelings about surgery, including reviewing the costs and benefits of the procedure;
- b. Examining your feelings of guilt, anxiety, deservingness, and entitlement and how these might affect your behaviors postoperatively;
- c. Thinking about the ways in which your relationship with food will change after the surgery and trying to identify strategies for filling the voids left by this change by incorporating gratifying and meaningful activities not related to food;
- d. Looking at the positive and negative aspects of your relationships with others to prepare an interpersonal stance that will allow you to hold on to healthy attitudes about your decision to undergo weight loss surgery no matter what others say.
- e. Planning in advance to share at least some of the above, including your anxious thoughts and feelings about any aspect of the surgery (including an untoward outcome such as death), with your significant others so that they can know in advance what you feel, what you need, and how they can help.
Conclusion
Hopefully, all will go well or has gone well, with your procedure. At this point, you are either still anticipating your surgery, or you have already undergone the procedure and are reviewing this material while recovering.
Before undergoing your surgery, it is helpful to identify those who will be able to care for you at various stages pre-and post-operatively.
For example, you should have a very detailed and well-developed list of individuals who will be available for you and the specific tasks that you would like to assign to them (of course, with their permission).
You will want to know well in advance who will transport you to the surgery, who will stay in the hospital while the procedure is completed, who will be there to visit you in the initial hours and up to a few days (assuming there are no complications) after, and what you would like various individuals to bring with them should you have needs of one type or another that could not be predicted in advance.
In preparing for what happens after you are discharged from the hospital, you will also want to know exactly who will “be there” for you in the hours, days, and weeks after you are at home following your surgery.

![Recipes for After Weight Loss Surgery [Detailed Guide 2021]](https://fatlossdudes.com/wp-content/uploads/2021/03/Weight-Loss-Surgery-Diet.jpg)
![Pre Weight Loss Surgery Diet [Complete Guide] – 2021](https://fatlossdudes.com/wp-content/uploads/2021/04/Pre-weightloss-surgery-diet.jpg)
![Bananas Benefits For Weight Loss: Literally You Can’t Believe [2021]](https://fatlossdudes.com/wp-content/uploads/2019/09/bananas-1354785_1920-min-768x512.jpg)
![[Top 15] Best Yoga Poses for Weight Loss – [2021]](https://fatlossdudes.com/wp-content/uploads/2021/03/Yoga-poses-to-lose-weight-768x432.jpg)
![Peptides: For Weight Loss, Benefits, Side Effects [2021]](https://fatlossdudes.com/wp-content/uploads/2021/02/what-are-peptides.jpg)
